CARTILAGE DEFECTS
Orthopaedic clinical problem
Chondrocytes are metabolically active cartilage cells that are responsible for developing, maintaining, and repairing the surrounding extracellular matrix
Cartilage defects can arise from daily wear, acute injury, degenerative conditions, or disease, resulting in pain, inflammation, and impaired joint function
Due to its avascular nature, articular cartilage has low metabolic activity, limited regenerative ability, and minimal self-healing capacity, making it especially difficult to repair
Injury triggers a cascade of biochemical and mechanical events that accelerate degeneration, potentially progressing to osteoarthritis (OA) and ultimately necessitating joint replacement if left untreated
PATHOPHYSIOLOGY
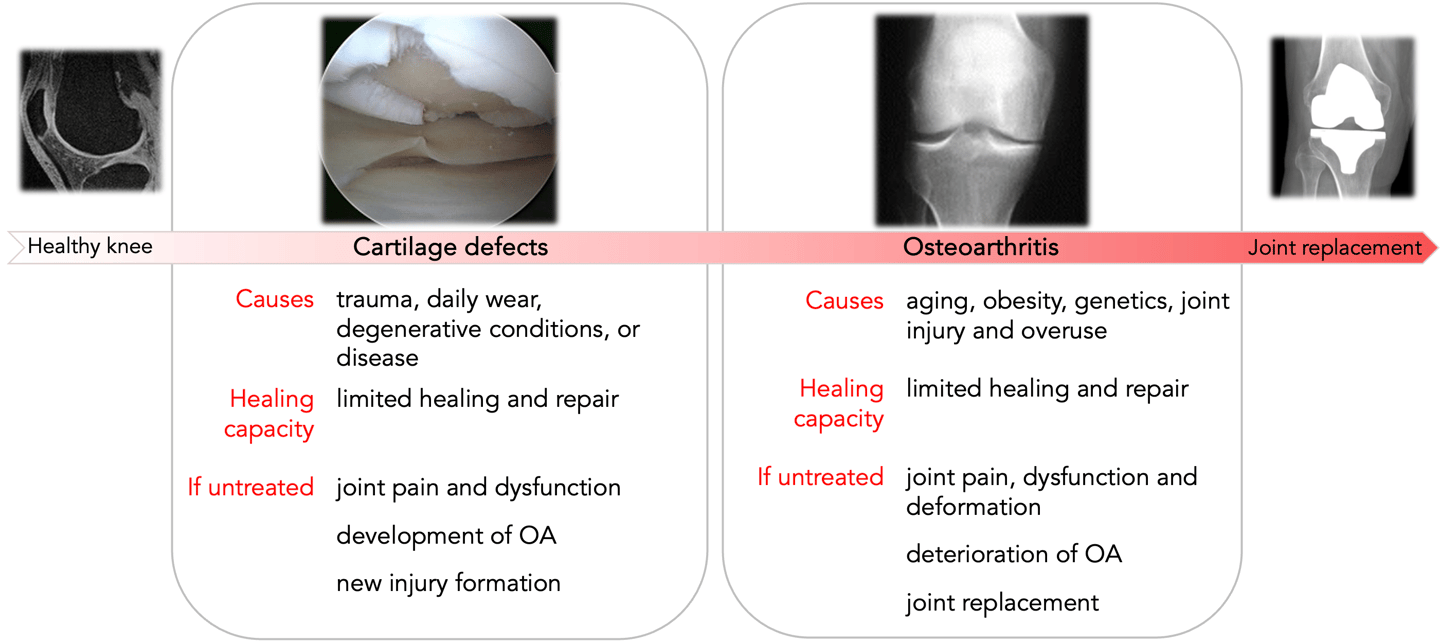
Early diagnosis and intervention with RECARTA can reduce the progression of cartilage defects
Microfracture has been considered the first choice cartilage repair over the last 20 years
LIMITATIONS OF CURRENTLY USED TECHNIQUES
42.1% reoperation rate at 2.63 years
fibrocartilage
subchondral sclerosis and cysts
intralesional osteophytes
severe bone marrow edema
Failure rates
11 – 27% within the first 5 years
6 – 32% at long-term follow-ups
>3.6cm² – predictive of additional surgical intervention in the future
Still lack of
standardized clinical evaluations
rehabilation protocols
radiological assessments
Reference: 1. W. Widuchowski, J. Widuchowski, T. Trzaska, Articular cartilage defects: Study of 25,124 knee arthroscopies, The Knee, Volume 14, Issue 3. 2007. 2. Orth P, Gao L, Madry H. Microfracture for cartilage repair in the knee: a systematic review of the contemporary literature. Knee Surg Sports Traumatol Arthrosc. 2020. 3. Weber, Alexander & Locker, Philip & Mayer, Erik & Cvetanovich, Gregory & Tilton, Annemarie & Erickson, Brandon & Yanke, Adam & Cole, Brian. Clinical Outcomes After Microfracture of the Knee: Midterm Follow-up. Orthopaedic Journal of Sports Medicine. 2018.


